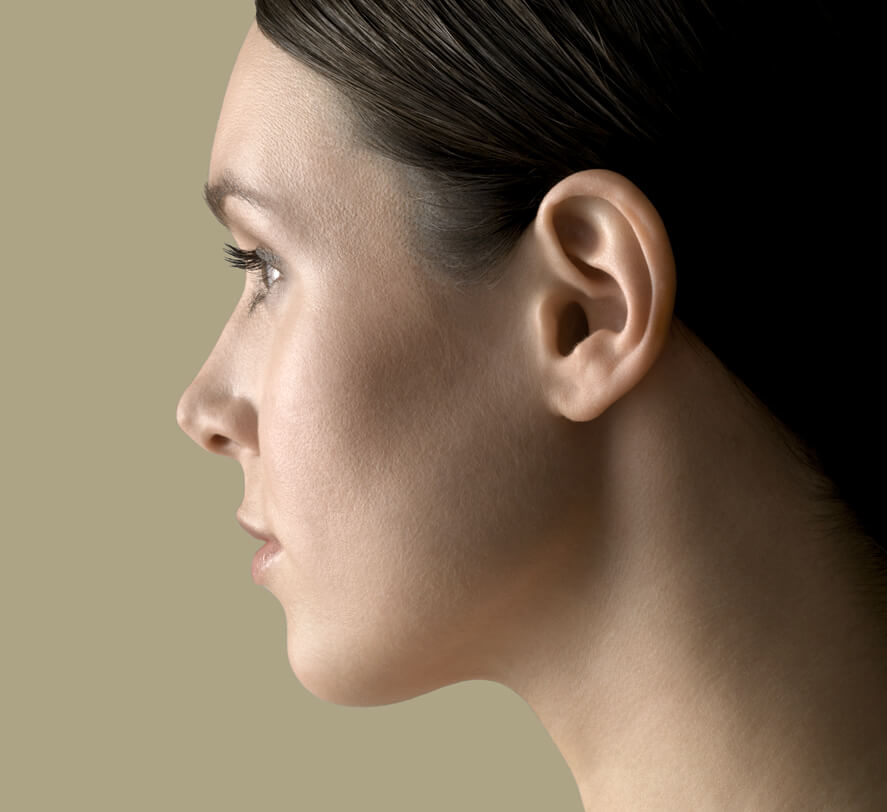
Protruding ears account for the most common congenital malformation in infancy. The cause of protruding ears is a deformity of the ear cartilage. In contrast to the Far East where protruding ears are often seen as a sign of wisdom and wealth, here in the West they are regarded as being strange. Many children with protruding ears are teased and called “Dumbo” at school. Feeling of shame and inferiority resulting from this can affect the self-confidence of a child. This can be avoided by a simple operation. Even in adulthood, protruding ears can be a visual distraction and can be a burden, which can be alleviated by an operation.
Like a fingerprint, every ear is uniquely shaped. Although ears come in a wide range of shapes and sizes, there is an ideal shape and size, as well as an ideal position. These norms guide surgical correction.
In general, there are two surgical treatments to correct the shape of the ear (otoplasty) or to correct protruding ears (otopexie). Otoplasty mostly involves both the correction of the shape and the position of the ear, which is why the terms otoplasty and otopexie are often used interchangeably.
Malformations of the ear can be corrected as early as 3 years of age, as at this age ears have already grown to 85% of their ultimate size.
Considerations
When to consider ear surgery:
- Ears protrude too far from the head
- Ears are asymmetrical
- Ears are to large
- Ears are dysplastic
The ear is normally positioned at an angle of 21–25 degrees to the head. A greater angle leads to the protrusion of the ear (apostasis otis) and can be caused by an enlarged ear cup (hyperplastic concha), an incomplete formation of the inner ear fold (hypoplastic anthelix) or a combination of both factors. Protruding ears are a mild form of ear malformation. In severe cases, the ear cup (pinna) is starkly malformed (“cup ear”) or the entire ear cartilage is incorrectly formed (ear dysplasia), too small (microtia) or even absent (anotia).
Mostly it is recommended to have the procedure performed before primary school starts (5–7 years old), to spare the child from teasing by classmates at school. However, it can be performed at any age as long as patient is healthy
Consultation
A prerequisite to a successful operation is careful planning. This starts with a personal consultation.
- Communication of wishes, expectations, ascertain what you would like to improve
- Explanation of the possibilities and scope of the operation
Examination:
- Medical history is taken
- Physical examination is performed
- Digital photos are taken
- Thickness, stiffness and malleability of ear cartilage is tested
To plan the operation and to make a risk assessment we require:
- Full medical history
- Allergies or aversion to medications
- Any important medical reports
Procedure
A variety of surgical procedures are available for the treatment of protruding ears. The appropriate procedure is chosen for you and your child. Ear shape is determined by the ear cartilage. Surgery focuses on correcting those parts of the ear that are malformed. The anthelical fold may be molded and the ear cup reduced and fixed closer to the head.
Reshaping of the anthelical fold can be made through an incision that is concealed in the external ear fold or on the back of the ear. Too large pinna can be reduced by an excision of ear cartilage or the ear cup can be rotated and secured closer to the head with sutures. Both procedures are performed through an incision behind the ear, where the scar is well hidden. In some instances with large ear cups, both cartilage and skin have to be removed from through an anterior approach. Some procedures involve correcting a protruding earlobe or reducing the size of an enlarged earlobe. Surgical correction of both ears usually requires a 1.5 to 2 hour operation. Depending on their age, children can have surgery performed under local or general anesthesia, as an inpatient or outpatient procedure. Adults generally have otoplasty as an outpatient procedure under local anaesthesia.
Risks
All operations carry risks. Thus, before every ear surgery there is a thorough discussion about general and individual risks. With any elective procedure the safety standards are even stricter than for a procedure that is medically necessary. The operation is carefully planned to minimize risks.
General risks from surgery include:
- Haematoma (bruising), bleeding and swelling
- Healing problems or infection
- Injury of deeper structures
- Numbness in the area of surgery (temporary or permanent)
- Circulatory problem of ear skin (skin slough)
- Scars
- Asymmetry
- Visible stitches, infection and perforation
- Relapse (recurrence) of ear deformity
- Unsatisfactory aesthetic result
- Secondary surgery
Overall, ear surgery is a safe procedure when undertaken by an experienced plastic surgeon and patients are mostly satisfied with the results. You or your child can help to minimize the risks by following the advice of your surgeon before and after surgery.
Preparation
Our aim is to make the time before and after the procedure as comfortable as possible. By following a few recommendations you can support our care:
- You or your child should not have a bad cold or be otherwise ill.
- To aid the healing process, avoid smoking for two weeks before and after the operation as smoking impairs healing.
- Avoid medication that increases the risk of bleeding, like aspirin, non-steroidal anti-inflammatory drugs, as well as vitamins and homeopathic remedies for two weeks prior to the operation.
- Ear surgery is mostly performed as an outpatient procedure under local anaesthesia. However, if you choose surgery to be performed under sedation or general anaesthesia, make sure that you can be collected and cared for by someone for 24 hours after the procedure.
Day of surgery
- Ear surgery in older children (>7 years) and adults can usually be performed on an outpatient basis under local anaesthesia at the AARE KLINIK.
- In younger children (<6 years) who don’t tolerate a local anaesthesia, the surgery is performed in hospital under general anaesthesia.
- During the operation various medications will be administered for the wellbeing of you or your child as needed.
- For your safety, your heart rate, blood pressure, oxygen supply etc. are monitored during the operation.
- After the procedure, the ears are protected by a special dressing, which should be worn for over a week until the sutures are removed.
- If the surgery is undertaken with a local anaesthetic, then you or your child can immediately leave the practice accompanied by someone.
- Instructions will be given as to what to do after surgery and what painkillers to take.
- After an outpatient operation your child should be at home under constant care for the first 24 hours.
- You will receive all necessary instructions for follow-up and advice in case of any unforeseen complications.
After surgery
- It is important to realise that recovery from an operation varies for every individual.
- During the first week after surgery you or your child should take it easy and keep your head and upper body in a raised position, sleeping on your back.
- Only take prescribed pain medication and do not take medication like aspirin.
- A head dressing is usually worn for a week.
- Small drains are removed 2 days after the operation.
- After removal of the head dressing, children should wear a headband for 2 weeks during the day and for 4 weeks during the night, until the ear shape has healed stably.
- Adults can usually get away with having nighttime protection from a headband for 7–10 days.
- Hair can be washed again once the bandage has been removed.
- Sutures are removed after 7–10 days.
- Avoid strenuous activities and sport for the first weeks after surgery.
- Avoid heat (e.g. bathing, sauna, solarium) for a few weeks until all swelling has subsided.
- Slight swelling and discolouration of the skin of the ears is normal in the first 1–2 weeks after the operation.
- Strong swelling or pain can be signs of a hematoma or infection and must be treated, otherwise irreversible damage can be caused to the skin of the ear and the ear cartilage.
- After surgery you will have numerous follow-up appointments until the final result is achieved.
Outcome
- The ears will be swollen, slightly discoloured and sensitive to touch for the first couple of weeks after the operation.
- Due to the healing process and swelling, it takes 2–3 months before the outcome of an operation can be fully evaluated and ultimately only after a year.
- Initially scars may be red and slightly thickened.
- Thick (hypertrophic) scars or keloids might require treatment with special silicone pads or cortisone injections.
- The result of otoplasty is generally permanent, however a recurrence can take place by the biological restoring force of the cartilage or the tearing of sutures.
- No ear is identical, therefore perfect symmetry of the ear shape and position is impossible to achieve.
- Pre-existing asymmetry of the head or ear cup, wound healing, or scar formation influence the result and can cause slight asymmetry even after otoplasty.
Costs
In childhood surgical treatment of protruding ears and other ear malformations are recognised and in individual cases costs may be carried by insurance companies. A cost estimate has to be made prior to surgery. In adulthood, otoplasty is mostly seen to be a purely aesthetic measure, in which case the costs are not carried by health insurance.
Costs of otoplasty vary depending on the scope and complexity of the surgery and where it is undertaken (AARE KLINIK/hospital) and can only be ascertained after a personal consultation.
The overall costs are made up of:
- Surgical fee (including consultation and post-operative care)
- Anaesthesia fee
- Technical infrastructure costs (AARE KLINIK/hospital)
- Inpatient hospital costs
- Medication
- Diagnostics (laboratory, ECG, scans, etc.)
Appointments for ear surgery with Dr. Scheufler in Bern
Before any ear surgery you should have a comprehensive consultation and additional examination. Only in this way can you be sure whether the type of surgery will lead to the result you expect. In addition, your consultation will give you a good impression of our experience in the field of facial surgery. Feel free to ask for before and after photos to get an idea of what the results look like.

Dr. med. O. Scheufler, specialist in plastic, reconstructive and aesthetic medicine and author of this website, is pleased to be at your service for a personal consultation. Besides his main work at the Aare Clinic, PD. Dr. Scheufler is also scientifically active and has habilitated at the University Hospital of Basel. He was therefore awarded the title of assistant professor by the University of Basel. In addition, he was honored by Duke University (USA) as a Visiting Professor. So do not hesitate to contact him if you wish a professional consultation!